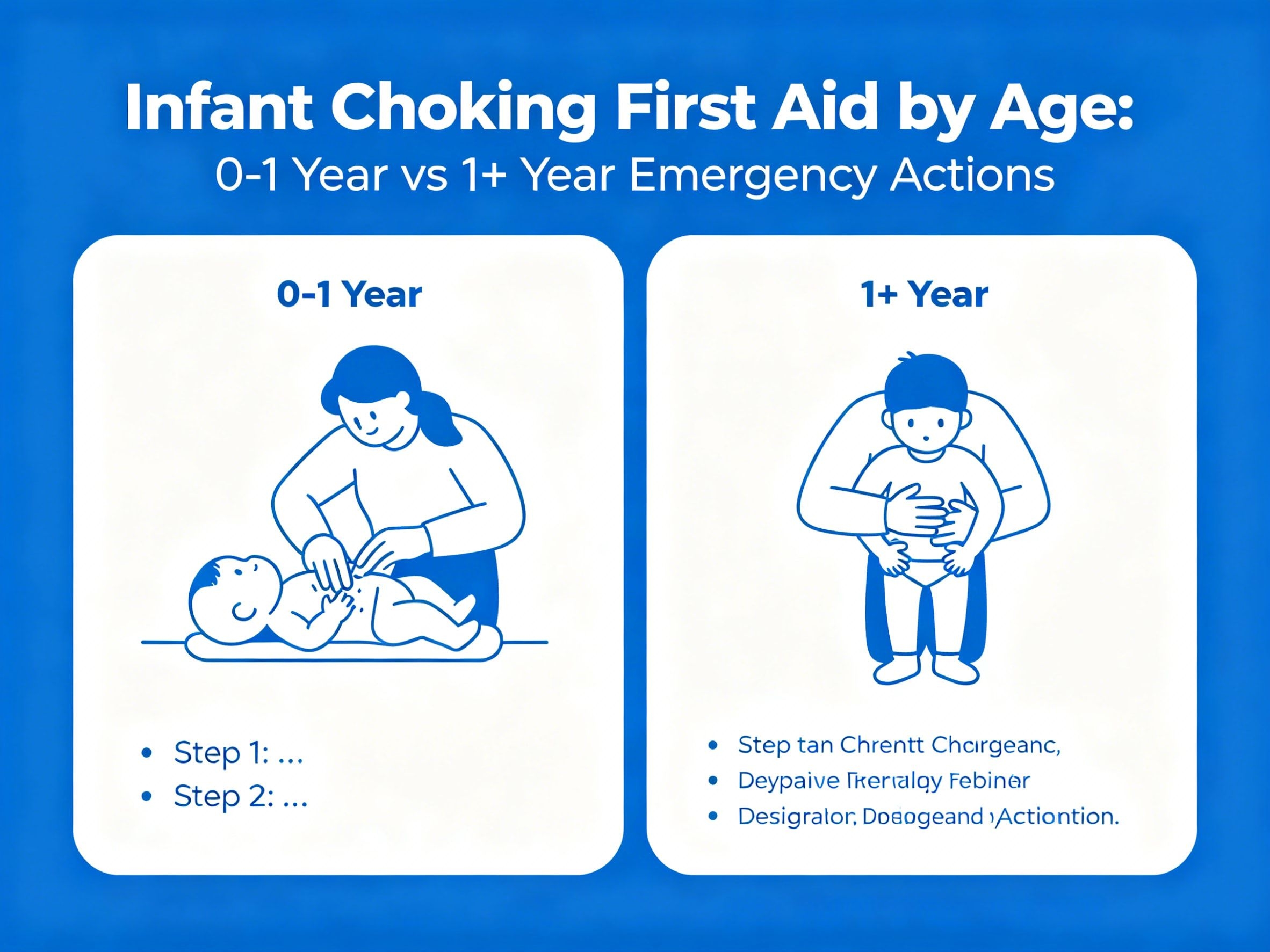
Infant Choking First Aid by Age: 0-1 Year vs 1+ Year Emergency Actions
- Published on
- //3 mins read/––– views
When a child chokes, seconds matter—and age-specific actions matter just as much. The first-aid sequence for infants under 1 year differs from the sequence for children over 1 year.
This guide is a safety overview for parents. It does not replace hands-on CPR/first-aid training.
Why age-specific choking actions are critical
Infants and older children differ in:
- airway size and anatomy
- force tolerance for rescue maneuvers
- recommended first-aid techniques
Using the wrong technique can delay effective care or increase harm.
Step 1: identify severe choking quickly
Possible severe choking signs:
- inability to cry/speak effectively
- silent or ineffective cough
- breathing difficulty, cyanosis, worsening distress
If the child is coughing effectively, encourage coughing and monitor closely.
Step 2: call emergency services early
If severe airway obstruction is suspected:
- call emergency services immediately (or have someone call)
- begin age-appropriate choking first aid
Do not delay emergency activation while trying repeated unstructured actions.
Infant under 1 year: core response principles
For infants, official first-aid guidance emphasizes age-specific positioning and alternating rescue techniques designed for this age group.
Key safety points:
- support infant head/neck correctly
- use recommended infant-specific sequence only
- avoid blind finger sweeps
- if unresponsive, begin CPR pathway per training while awaiting emergency responders
Child over 1 year: core response principles
For older children, guidance shifts to age-appropriate abdominal/chest rescue maneuvers and CPR transition if unresponsive.
Key safety points:
- use child-appropriate technique and force
- avoid blind finger sweeps
- activate emergency help early
What never to do in choking events
- do not do blind finger sweeps
- do not shake or invert child aggressively
- do not give food/water “to push it down”
- do not wait too long if breathing is compromised
Common parent confusion points
“Strong cough means I should intervene immediately with maneuvers”
If cough is effective and child is moving air, encourage coughing and observe closely.
“If object seems gone, no follow-up needed”
Persistent cough/noisy breathing after event may require evaluation.
“I can learn this only from short social videos”
Hands-on accredited training is strongly recommended.
After the event: when to seek urgent review
Seek urgent medical assessment if:
- breathing remains noisy/difficult
- cough persists abnormally
- any unresponsive period occurred
- you are uncertain whether complete airway clearance happened
Family preparedness checklist
- complete infant/child CPR and choking course
- post emergency numbers visibly
- align all caregivers on same response protocol
- refresh training regularly
FAQ
Is infant choking response the same as for a toddler?
No. Techniques differ by age and must be applied correctly.
Should I try to pull object out with my fingers?
Not blindly. Blind sweeps can worsen obstruction.
Can I wait and see if severe choking resolves?
No. If breathing is compromised, call emergency services immediately.
What is the most useful prevention step?
Caregiver training plus food/environment choking-risk control.
References
- NHS: How to stop a child from choking
- American Red Cross: Infant choking
- AHA/AAP update on CPR guidance
- AAP HealthyChildren: Choking prevention
- MedlinePlus: Choking infant under 1 year
Final takeaway
In choking emergencies, act fast and use age-correct techniques: infant and child pathways are not interchangeable. Early emergency activation and trained response save lives.

