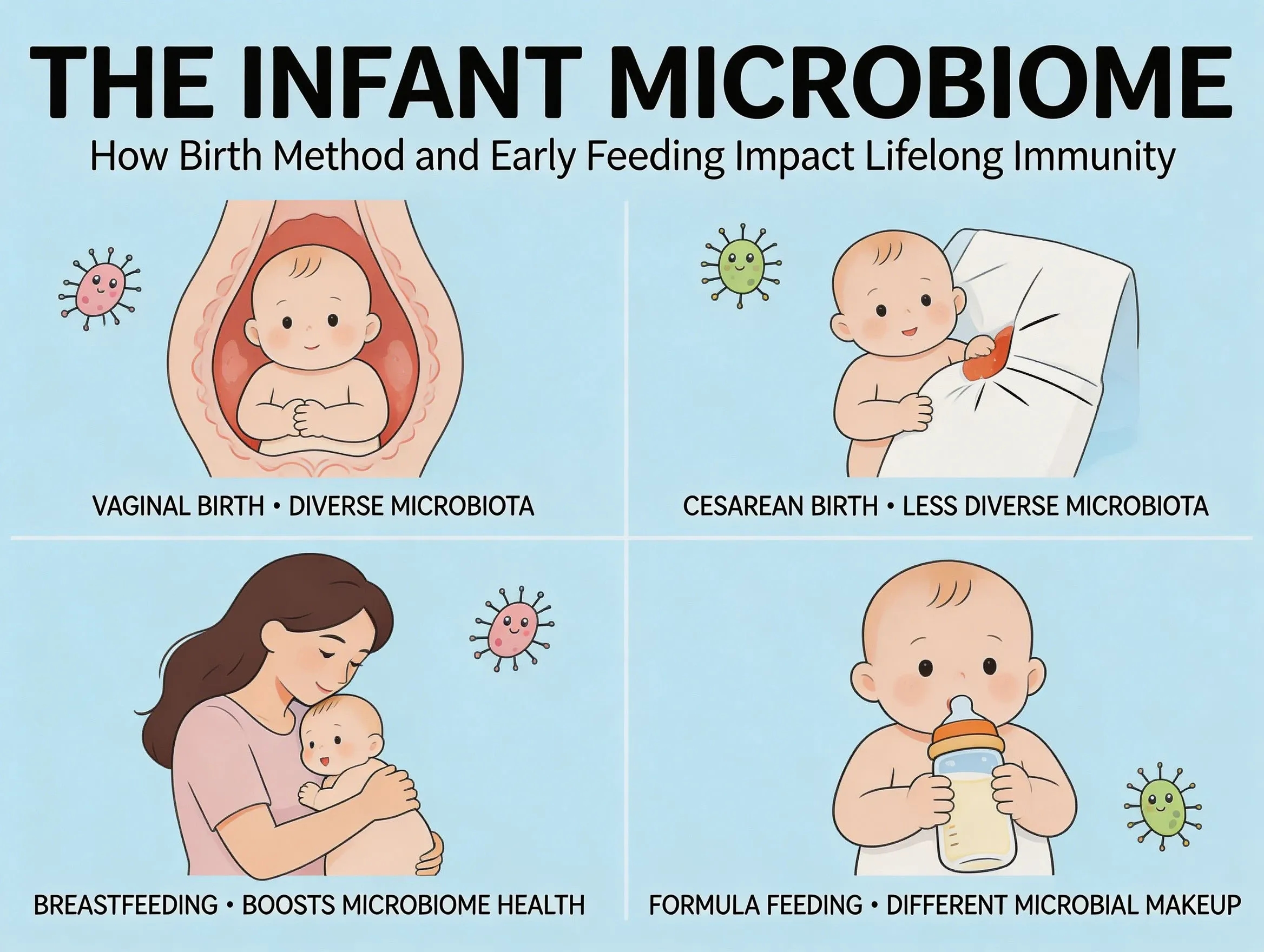
The Infant Microbiome: How Birth Method and Early Feeding Impact Lifelong Immunity
- Published on
- //6 mins read/––– views
The first months of life are not just about growth charts and sleep schedules. They are also a period of intense biological programming, including the formation of the infant gut microbiome—an ecosystem that helps train metabolism, barrier function, and immune development.
Parents often hear simplified claims online: "C-section permanently damages the microbiome" or "formula ruins immunity." These statements are not only emotionally harmful, they are scientifically incomplete.
This guide explains what evidence supports, what remains uncertain, and how to make practical decisions without shame.
What is the infant microbiome, and why immunity depends on it
The infant microbiome is the community of microorganisms that colonizes the baby’s body, especially the gut. In early life, this ecosystem interacts with immune cells, influences inflammation pathways, and helps calibrate immune tolerance.
Think of it as an early training environment rather than a single "good vs bad" score.
Important: microbiome development is dynamic. It changes with feeding, medications, infections, environment, and age.
Birth method and microbiome seeding: what we know
Vaginal birth and early colonization
Vaginal birth is associated with early microbial exposure patterns different from cesarean birth. These differences are measurable in the newborn period.
Cesarean birth and early divergence
C-section birth often shows distinct early microbiome composition. However, newer data suggests trajectories can converge over time, and many modifiers (especially feeding pattern) influence outcomes substantially.
Avoiding overclaim
A different early profile is not a destiny sentence. It is one biological context among many.
Early feeding as a major microbiome and immune modifier
Human milk and immune-active components
Human milk contains bioactive compounds—including human milk oligosaccharides (HMOs)—that selectively support beneficial microbial ecosystems and immune signaling.
Exclusive breastfeeding guidance and public health consensus
Major authorities (WHO, CDC, NHS, AAP) consistently emphasize breastfeeding as an important infant health strategy, including infection protection and immune support.
When exclusive breastfeeding is not possible
Mixed feeding, donor milk contexts, medically indicated formula use, and individualized plans are common real-world situations. The objective is not perfection; it is safe, sustained nutrition and responsive pediatric follow-up.
Birth method + feeding pattern: the interaction matters most
One of the most useful updates from recent research is that single-factor narratives are weak.
A practical interpretation:
- Birth mode can shape early microbial starting patterns.
- Early feeding can strongly influence microbial direction afterward.
- Clinical outcomes depend on the broader context (gestational factors, antibiotics, home environment, illness exposures, and social determinants).
So parents should think in systems, not blame.
What "lifelong immunity" really means (without exaggeration)
It is accurate to say early-life microbial and feeding exposures are linked to immune development pathways. It is not accurate to promise deterministic long-term outcomes for an individual child based on one input alone.
Use this safer wording model:
- Accurate: "Early microbiome and feeding patterns are associated with immune trajectory."
- Overclaim: "This birth/feeding choice guarantees future disease risk."
Practical, no-guilt actions for families
1) Prioritize safe feeding continuity
Whether breastfeeding, mixed feeding, or formula feeding, consistency, growth monitoring, and pediatric review matter.
2) Protect follow-up after cesarean birth
If baby is born by C-section, focus on evidence-based postnatal care: feeding support, skin-to-skin when feasible, and regular pediatric assessment.
3) Be careful with unproven hacks
"DIY microbiome fixes" and social media protocols can outpace evidence. Discuss any supplements or interventions with clinicians.
4) Track whole-child health, not one biomarker
Weight gain, feeding comfort, stool pattern changes, infection history, and developmental progress together are more meaningful than isolated internet interpretations.
Common misconceptions parents should ignore
Misconception 1: "C-section babies have permanently damaged immunity"
Evidence does not support this absolute claim.
Misconception 2: "Only exclusive breastfeeding creates a healthy microbiome"
Breastfeeding has strong benefits, but infant health is multifactorial; many children thrive under different medically appropriate feeding paths.
Misconception 3: "Microbiome test kits can tell me my baby’s future"
Current consumer microbiome tools have limited predictive power for individual long-term outcomes.
Misconception 4: "One feeding decision determines lifelong disease"
Science supports associations and risk modulation, not certainty for individual destiny.
Parent-friendly fact-check checklist for microbiome claims
Before trusting a headline, ask:
- Is the source an established health authority or peer-reviewed journal?
- Does the claim separate association from causation?
- Is study context clear (population, follow-up length, confounders)?
- Does it avoid fear-based deterministic wording?
- Does it include practical guidance rather than guilt messaging?
If the answer is mostly "no," treat the claim as low reliability.
FAQ
Does cesarean birth automatically mean weaker immunity?
No. Cesarean birth can influence early microbiome patterns, but child immune development depends on many interacting factors.
Is breastfeeding the only path to good immune outcomes?
Breastfeeding offers important benefits, but when it is not exclusive or not possible, safe alternatives and consistent pediatric care still support healthy outcomes.
Should parents try unverified microbiome interventions at home?
No. Use clinician-guided strategies and avoid interventions that outpace evidence.
What should parents focus on first in the newborn months?
Reliable feeding, growth monitoring, vaccination on schedule, infection-awareness, and timely pediatric follow-up.
References
- WHO: Breastfeeding (health topic)
- WHO Fact Sheet: Infant and young child feeding
- UNICEF Data: Breastfeeding
- UNICEF Data: Breastfeeding dataset
- CDC: Breastfeeding recommendations and guidance
- CDC: Breastfeeding benefits both baby and mom
- NHS: Benefits of breastfeeding
- AAP Pediatrics (2022): Breastfeeding and the use of human milk
- PubMed (2024): Delivery mode as determinant of infant gut microbiome at 6 weeks
- PubMed (2024): Effect of delivery mode on intestinal microbiota and immune function of neonates
- Frontiers (2024): Delivery mode and neonatal initial gut microbiota
- Frontiers in Immunology (2024): Interactions of human milk oligosaccharides with the immune system
- PubMed (2024): HMOs and Bifidobacterium in infant intestinal protection
Final takeaway
Birth method and early feeding do influence early microbiome development, but no single decision writes your child’s future alone. The strongest strategy is evidence-based feeding support, regular pediatric care, and rejecting fear-based overclaims.

